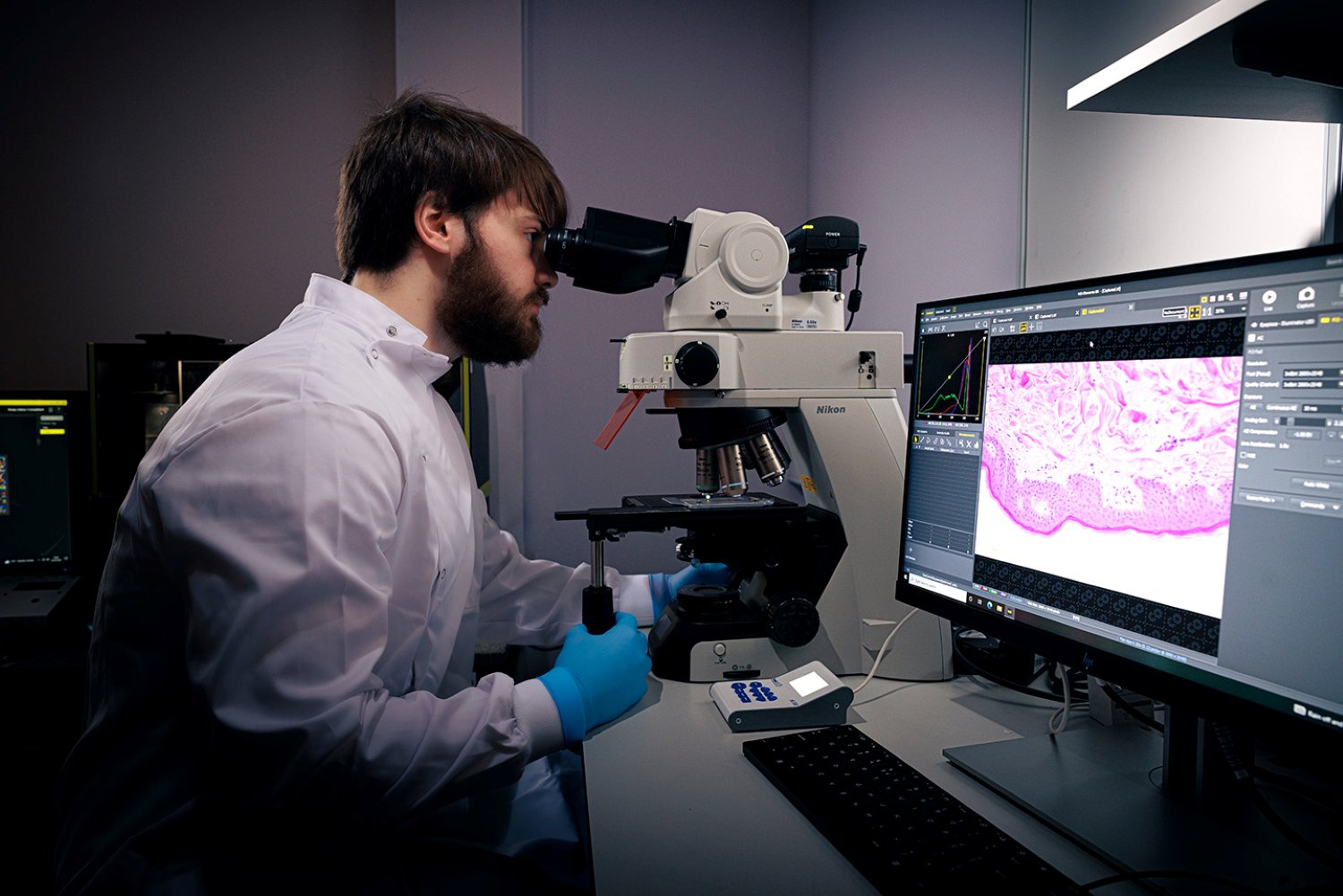
Chronic wounds can arise after operations, amputations and as part of long-term conditions like diabetes, and cost the NHS £8.3 billion annually.
That’s more than cancer and obesity.
Now, the University of Hull’s £48 million Wound Innovation Institute will create new treatments to reduce pain and suffering.
With investment from UK Research and Innovation, it brings together world-leading discovery science, clinical expertise and industry collaboration.
Freeing up NHS resources
Science Minister, Lord Vallance, said:
People living with chronic wounds that fail to heal are forced to struggle on in distress and discomfort.
That’s why we are determined to support new innovations to deliver a health service which is fit for the future, improves lives, and delivers real impact for people.
The new Wound Innovation Institute in Hull will help us do exactly that; allowing clinicians and industry to pioneer treatments which heal wounds faster, improve outcomes after surgery, and free up more resources for our NHS to do what it does best.
Better care, faster recovery
Professor Matthew Hardman, Director of the Wound Innovation Institute, said:
For too long, chronic wounds have quietly cost the NHS billions and devastated quality of life.
The Wound Innovation Institute exists to change that.
We’re delivering world leading research that translates directly into better care, faster recovery and easing pressure on NHS services.
The University won a £16 million bid from the UK Research Partnership Investment Fund to establish the national facility, with matching funded by industry partners including Polaroid Therapeutics and Reckitt.
The investment allows universities to develop ground-breaking research infrastructure to tackle our biggest research challenges.
The invisible burden
Professor Dame Jessica Corner, Executive Chair of Research England, said:
Chronic wounds represent a huge and often invisible burden on patients and the NHS alike, and this Institute brings together the scientific excellence, clinical partnerships and industry collaboration needed to make a real difference.
The University of Hull has built something genuinely transformative here, and I’m proud that the UK Research Partnership Investment Fund is helping to turn world-leading research into better outcomes for millions of people across the country.
Supporting healing
Current research projects include:
- focusing on the skin microbiome, the community of bacteria living on the skin, and its role in protecting against infection and supporting healing
- uncovering why older people and those living with diabetes are far more likely to develop wounds that fail to heal, and how specific harmful bacteria drive poor outcomes
- using cutting‑edge genomic technologies and working with NHS clinicians to show how targeted therapies could replace antibiotics, to improve healing, tackling the growing threat of antimicrobial resistance
- understanding exactly how healthy skin protects us and what changes when wounds fail to heal, so that researchers can develop more precise, effective treatments that prevent infection and support recovery
Help for people with amputations
Research also has the potential to reduce hospitalisation, prevent amputations and transform recovery after limb loss, where delays often slow rehabilitation.
Following a below‑the‑knee amputation, patients are usually fitted with a prosthetic limb.
However, in the first year after surgery their limb changes shape rapidly and prosthetic sockets can’t adapt, often becoming painful or unusable.
This forces patients to wait weeks or months for replacements.
In response researchers are testing a heat‑remouldable prosthetic socket that can be fitted in a single session and reshaped as the limb heals, reducing delays, clinic visits and discomfort.
Using ultrasound
Scientists are also identifying innovative new treatments using ultrasound to promote healing of diabetic foot ulcers.
An estimated 90,000 people are living with painful foot ulcers that affect their ability to walk, to work and may lead to lower limb amputations.
Ultrasound therapy can accelerate healing and reduce costs over conventional treatments.
Further information
Help for people with amputated limbs
A remouldable socket has the potential to improve comfort during rehabilitation, reduce waiting times, and help patients begin walking sooner.
One such device, the Confidence Socket, developed by project partner Amparo Prosthetics, is already demonstrating these benefits in the real world.
It has already been used in humanitarian settings, including during the war in Gaza.
Its ability to be made and fitted in a single session, even in challenging surroundings, has enabled patients to receive immediate, effective care.
Working with Amparo and the NHS, the researchers are leading a new study, ASSIST, to investigate whether a remouldable socket can help patients recover quicker and reduce waiting times.
Patients with lived experience of limb loss have shaped the study from the start, ensuring it reflects real world priorities and experiences.
Focusing on people with diabetes
Living with chronic wounds significantly reduces quality of life for 2.2 million people across the UK, with people with diabetes and older people particularly likely to be affected.
Patients often experience pain, odour, social isolation and depression.
Skin is our largest and most intricate organ, protecting us from harmful germs through sophisticated defence systems and complex microbial communities.
Yet research into how the skin microbiome works is in its infancy.
So, we’re investigating how age and diabetes cause poor healing by uncovering how the skin interacts with its microbial defence system, the microbiome.
We’re delivering breakthrough insights into how the microbiome maintains healthy skin, driving the development of more effective wound care.
Rising antimicrobial resistance further complicates wound care, demanding innovative solutions to replace broad-spectrum antibiotics.